Odette Aoife W.
Born: 10/21 at 12:33am
Weight: 6lbs 14.8 oz
Height: 19.25 in
NATURAL BIRTH STORY from Mom’s perspective
I was due on October 9th. Well, October 9th came and went, to our shock, because I had experienced preterm labor at 29 weeks. (We’d spent the night in the hospital to get contractions to stop and when we were told we could go home, they put me on quite the restricted regimen. No working out, very little work, no more travel, etc.) All that to say, we were expecting our baby to be early.
A Promise of No Induction Talk Until 41Weeks
As we approached my due date, we started talking with my doctor about what would happen, should I be overdue. Since she knew I wanted a natural birth, she said she’d let me go to 42 weeks and she said she’d let me hit 41 before talking about any type of induction.
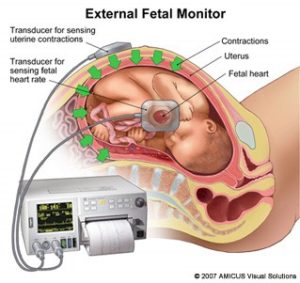
Non-Stress Testing Begins
At our 40week appointment she started doing an amniotic fluid check and non-stress tests. Baby looked good, so we kept going, hoping for a natural birth. We really wanted to trust the whole process.
Really Wanted to Avoid Induction
At 41 weeks I allowed her to check my cervix for the first time because she started talking about induction methods and she kept saying “without a check I can’t offer my best professional opinion about how far to let you go or how we should induce if we need to”. I really didn’t want to be induced and thought that if she could check my cervix and see what was going on she’d be up for giving me more time. I really trusted that my body was working on things and leading me toward my natural birth. Sure enough I was 2-3cm dilated and 80% effaced. She said I could go “at any minute” but if I didn’t, she wanted to sweep my membranes in two days.
Pressure On!
Two days later (on a Friday) we were back in the office, still waiting for labor to begin on its own. I was now 3cm dilated and 90% effaced at 41 weeks and 2 days. She said we should sweep my membranes and labor would start. I asked her if I could have the weekend to see if my body would kick things off on its own. I was still determined to trust the process and have my natural birth. She pushed back and said “there was no downside to a membrane sweep”. I disagreed*. [The risks to membrane sweeping/membrane stripping are: premature rupture of membranes (breaking the amniotic sac) leading to infection, bleeding, irregular contractions, discomfort during vaginal exam, may not always lead to labor starting] I knew it would possibly start the intervention domino effect and I wanted more time. She agreed to give me the weekend but said, come Monday at 41 weeks 5 days we’d do the sweep.
Advocate for Myself and My Baby
I really felt like I had to push for what I wanted. And I’d felt supported by my doctor through my entire pregnancy, so it was hard to push back on what she wanted to do. When I asked why for the membranes sweep so early in week 41 when she’d previously told me I could go to 42 weeks, she’d only say, “well this is what we do”, or “there’s no downside to a sweep,” despite the fact that my amniotic fluid looked really good and so did my non-stress tests. It was an emotional place to be in for the week, wanting to advocate for my body, my baby, and myself while second guessing everything based on my doctor’s reaction and what she wanted to do.
Natural Induction Techniques
Well we took the weekend to try to coax the little one out using natural induction techniques. We tried everything on Liza’s handouts from our Bradley Method childbirth class. We even hopped on the phone to talk to Liza about things. She suggested I pump for longer than I had been. On Sunday I went for a 4.5 mile walk and pumped for two hours from 4:30pm-6:30pm. I started having contractions at 6:30pm.
See Related Post: 9 Ways to Do Nipple Stimulation
We’re in Business!
I immediately knew that things were starting, if they’d only keep going we’d be in business. The contractions felt like intense period cramps to start and I was able to eat and laugh with Caleb in between them for about an hour and a half. Things got intense quickly from there. My doula told us on the phone to put me in bed so I could get some sleep but I already knew things were moving faster than that. There was no way I could sleep through what was happening.
Caleb, My Anchor
I don’t know the time frame as well as Caleb, but I needed to really prepare my breath for each contraction. If I didn’t, I’d tense up and feel like I was losing control and feel the pain was running away with me. If I breathed before it started and through it, it went much better. I also needed Caleb to be touching me in some way. His touch was like an anchor for me, keeping me focused. The few times he had to walk away from me to get or do something, I felt as though the pain carried me away and I couldn’t control it, his touch kept me grounded.
Need to Move!
I was only comfortable on the exercise ball, moving my hips in circles and from side to side. I eventually leaned over our kitchen counter and collapsed in between contractions to rest while still sitting on the ball. I tried for a round of contractions getting into the side lying pose for relaxation and it was hell. I needed to move. Simply laying there felt like I was a victim to the pain.
Guided by the Doula’s Knowledge
After Caleb got off the phone with our doula she recommended belly sifting and belly lifts in the shower and then to call her after. We did both of those things and then I wanted to just stay in the shower with water running over me and moan through the pain. I basically had my eyes closed the whole time. At some point the doula arrived and she must have seen how quickly things were moving because she got me out of the shower (which was tough, I didn’t want to get out) and she put me on the toilet straddling it backwards and laying over the tank. The contractions were getting more and more intense, the pressure was almost unbearable. And then just as I had the thought that I couldn’t stand it anymore, my water broke. I had some minor relief for a small window of time and my doula must have been familiar with that window because she said “Jen, you’re gonna get a small break here, let’s get you dressed and downstairs and in the car”.
Intense!
In the car things got even more intense and I felt the urge to push. I kept my eyes closed and resisted the urge as much as possible. When we got to the hospital I collapsed in the hallway on the way to our room because the pressure in my pelvis wouldn’t allow my to walk. I felt her descending into the birth canal and continued to resist the urge to push.
Time to Push
They immediately checked my cervix and told me I was 9cm dilated and by the time they’d gotten me in a gown and on an IV for fluids I was telling Caleb and my doula I wanted to push. The doc checked me again and said that I was ready at 10cm. Pushing gave me something to do. And while I wouldn’t say I looooooved the sensation, it felt productive. I pushed for 45 min and our baby girl was born at 12:33am on October 21st. I had a couple stitches and delivered the placenta without issue. I was up and moving around after that golden hour of skin to skin. I felt very present, aware, and awake after she was born, and while I’ve been sore recovery overall has gone VERY well. My favorite things are the “padsicles” that I made myself before she was born.
We’re all doing really well and are happy and healthy.
And now for Dad’s Perspective…
BIRTH STORY from Caleb’s perspective
It all happened so fast, but being almost 2 weeks past the due date Jen (and her body) were ready.
(6:30pm to 8:30pm) Early Labor
The first 60 minutes of contractions Jen could handle mostly on her own and would look at me normally and talk to me or finish eating dinner in between. Because Jen was already so late, 3 cm dilated, and 90% effaced our doctor told us to go to the hospital once she started have 1 minute contractions, 5 minutes apart for 1 hour[for most people this is too early]. Well, that’s what happened in the first hour… and I didn’t see a transition from Jen yet, so we waited.
Focused
Another hour of contractions at 1 minute long, 5 minutes apart and Jen was starting to turn more inward and needed me to rub her back or put pressure on the outside of her hips. During rest times she would keep her eyes closed and just breath. Not really talking to me. We tried to switch it up and have Jen lay on her side, but after trying through 3 contractions, she hated it. ¯\_(ツ)_/¯
(8:30pm to 10:30pm) Communicating with the Doula
I had been texting with the doula, but the next intense 2 hours made me feel the need to call the doula at 8:53pm. She talked to Jen, encouraged her to do 15 minutes of belly sifting and 10 contractions worth of ab/belly lifts in the shower and then call her. By the 9th, Jen couldn’t stand on her own. She was moaning a lot throughout. (Sorry neighbors! Although they swear they couldn’t hear…)
Jen in “Labor Land”
I would describe Jen as being in a focused trance. She was “there”, but in the flow of what her body was doing. During the rest periods she would basically collapse. I had been timing the contractions through all of this and they were 60 to 70 seconds long, on average of 3 minutes apart, for over an hour. We called the doula and asked her to come over at 9:42pm. While we waited, Jen labored on a smaller birth ball in the shower with the wand running hot water over her.
(10:30pm to 11:15pm). Active Labor
Within a few minutes of the doula arriving we moved Jen from the shower to sitting backwards on the toilet because she was feeling a lot of pressure. Our doula was asking if her water broke in the shower and neither of us thought it did. While on the toilet, the doula looked at me and said something along the lines of “do you have everything packed and ready to go?” I said “almost”, and went around the house grabbing the last things and put them in the car. When I came back up, Jen’s water broke on the toilet, which relieved some of the pressure for her. We then started to get ready to leave for the hospital.
At the Hospital
Once in the car, we drove 8 minutes to the hospital, through a few contractions, trying not to push, and we checked in. On the way from the L&D front desk to the room (probably 50 feet) Jen basically collapsed into our arms. Her knees buckled and she couldn’t walk anymore. We wheelchair her into the room and things got going.
(11:15pm to 12:33am). Transition
Once in the hospital room, Jen contractions were so intense that we had to tell the nurses to wait to “hook her up” to anything until she was in between them. Jen just sat on the edge of the bed through 1 or 2 of them. They checked her right away and she was 9cm, so they told her to wait and not push. They started monitoring, put in an IV hole, but no drip. After a few more contractions, they had Jen lay her back down on the bed so the midwife could check again. She was 10 cm and -1.
Time to Push
Jen first tried pushing laying on her side for 5 contractions I’d say. A little bit of progress was made that way. They gave Jen an oxygen mask. She then switched to on her back holding her knees up to her chest. Our Doula held one leg, a nurse and I held the other and Jen pushed through 7 to 10 contractions before our daughter was born all in one push. Head, shoulders, everything.
So Proud of My Amazing Wife! 
Jen did so amazing. Our doula was so great leading up to and especially right during/after the birth. I can’t imagine it going any better for Jen, who really wanted a natural birth. I’m so proud of her. We went home from the hospital Wednesday afternoon. About 39 hours after Odette’s birth.